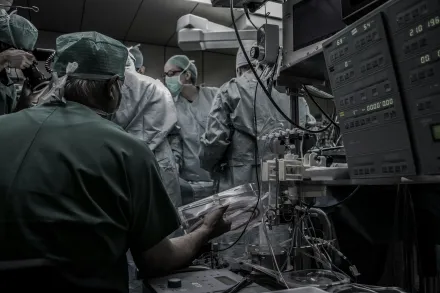
In many surgical disciplines robotics has emerged as a pivotal technology that reshapes how surgeons approach complex anatomy, especially in the thoracic cavity where access is often limited and precision is paramount. The field of cardiovascular surgery stands as a notable example of how robotic assistance can extend the reach of skilled hands while reducing the physical footprint of traditional approaches. The integration of robotic platforms brings together advanced visualization, meticulous instrument control, and enhanced ergonomics to support procedures that demand delicate tissue handling, precise suturing, and rapid adaptation to evolving intraoperative circumstances. This shift is not merely about adopting a new tool, but about reimagining procedural workflows, refining patient selection, and coordinating multidisciplinary teams to deliver safer, less invasive interventions with faster recovery. As clinicians and engineers collaborate, the role of robotics continues to evolve from experimental adjunct to a standard consideration in carefully chosen cases, driven by outcomes, patient preferences, and the economics of modern health care.
Historical context and evolution
Robotics in cardiovascular surgery began as an offshoot of broader surgical robotics, with early explorations focused on translating expert movements into precise actions within confined chest excursions. The initial decades of development were characterized by cautious experimentation, small case series, and a slowly expanding repertoire of indications. Surgeons and engineers worked to overcome fundamental barriers such as achieving stable visualization, controlling instrument motion with high fidelity, and addressing the absence of tactile feedback that is intrinsic to open surgery. Over time, the emergence of three dimensional high-definition imaging, motion scaling, tremor filtration, and wristed end effectors markedly improved the ability to navigate around critical structures such as the mitral apparatus and coronary targets. As experience accrued, centers cultivated standardized protocols for patient selection, anesthetic coordination, and intraoperative imaging integration, enabling a more predictable workflow and safer execution of robotic-assisted cardiac procedures. The trajectory from exploratory cases to more routine adoption reflects a maturation process driven by cumulative lessons, iterative hardware improvements, and a growing body of clinical data that guided best practices in coordination and safety.
Robotic platforms and instrumentations
Modern cardiovascular robotic systems provide teleoperation from a surgical console, where the surgeon controls a set of articulated arms equipped with EndoWrist instruments that replicate and extend the natural range of motion. These devices enable precise needle driving, fine tissue dissection, and accurate suture placement within the small corridors of the thoracic cavity. The visualization pipeline delivers high-definition, magnified, three dimensional imagery that enhances depth perception and spatial awareness during complex maneuvers such as leaflet resection, chordal repair, and annular reconstruction. Motion scaling and tremor reduction further refine precision, allowing surgeons to perform intricate tasks with a level of control that is challenging to achieve with conventional instruments through small thoracotomies. While tactile feedback remains an area of active development and debate, teams compensate with enhanced visual cues and meticulous technique, combined with close communication with the bedside assistant. The platforms are designed to be adaptable to various cardiac procedures, with instrument configurations that support dissection, suturing, stapling, and fast exchange of specialized tools. In practice, robotics is often integrated with intraoperative imaging modalities, including transesophageal echocardiography and computed tomography guidance, to verify alignment, measure annular dimensions, and confirm graft or prosthesis seating in real time, which helps reduce the likelihood of postoperative complications related to misalignment or inadequate repair geometry.
Applications in cardiac and vascular surgery
Within the spectrum of cardiovascular surgery, robotic assistance has demonstrated meaningful value in procedures where access through a full sternotomy would entail greater morbidity. In mitral valve surgery, robotic approaches have facilitated complex repairs that require precise leaflet resection, chordal replacement, and annular stabilization, enabling high-quality repairs through minimized incisions and preserved chest wall integrity. The ability to manipulate delicate valve tissue under magnified visualization can contribute to durable repairs, with potential implications for freedom from reoperation and improved functional outcomes. Similarly, robotic assistance has expanded capabilities for tricuspid valve repair when approached from a right thoracotomy or a left-sided port configuration, allowing targeted reconstruction while often avoiding sternotomy. In coronary surgery, robotic systems enable minimally invasive bypass grafting techniques, including small chest incisions that permit targeted anastomoses to the left anterior descending artery or other targets, sometimes in hybrid configurations that combine robotic exposure with endoscopic harvesting of conduits. Pediatric and congenital cases have also benefited in selected scenarios, where precise access and constrained anatomy demand enhanced visualization and careful tissue handling. Across these applications, successful robotic procedures rely on meticulous patient selection, rigorous preoperative planning, and a shared mental model among cardiovascular surgeons, anesthesiologists, imaging specialists, and perfusion teams to ensure synchronized execution and complication readiness.
Procedural techniques and workflows
Most robotic cardiovascular procedures require a carefully choreographed sequence that begins with thorough preoperative assessment and planning, including high-quality imaging to delineate anatomy and plan port placement. Intraoperative steps typically involve establishing a stable operative field through cardiopulmonary bypass or beating-heart strategies, followed by docking the robotic arms to strategically positioned ports that optimize exposure of the target structure. Stabilization devices and adjuncts are employed to minimize motion of the heart during suturing and reconstruction, while the surgeon at the console performs precise dissection, tissue manipulation, and valve reconstruction with suturing technique that benefits from magnified visualization. The workflow emphasizes gentle tissue handling, progressive exposure of the operative site, and real-time communication with the bedside assistant, particularly when tasks require rapid instrument exchange or hemostasis. The ability to convert to a conventional sternotomy remains a critical safety option if unexpected complexity arises, and established protocols exist to facilitate a safe and timely transition. Across institutions, the standardization of steps—from port placement to intracardiac manipulations—has contributed to more predictable operative times and improved adherence to quality metrics, even as each case presents unique anatomical and physiological challenges that demand on-the-spot clinical judgment.
Patient outcomes and clinical evidence
Clinical experience in robotic cardiovascular surgery has consistently highlighted trends toward reduced surgical invasiveness, with benefits including smaller chest wall trauma, decreased transfusion requirements, reduced postoperative pain, shorter intensive care stays where feasible, and shorter overall hospitalization. In valve procedures, robotic repairs and reconstructions have shown encouraging durability in experienced hands, with some series reporting favorable rates of successful repair and acceptable long-term function paralleling traditional approaches. For coronary bypass, robotic assistance can offer targeted revascularization with a less extensive thoracic disruption, potentially translating into faster recovery for select patients. It is important to acknowledge that reported outcomes vary by procedure, patient selection, and institutional expertise; higher-quality, multicenter data remain essential to generalize findings and to clarify the balance between perioperative risk, learning curves, and long-term durability. As the evidence base matures, registries and collaborative studies contribute to refining indications, optimizing protocols, and informing patient counseling about expected benefits and potential risks associated with robotic technologies in cardiovascular care.
Technical considerations and challenges
Several technical realities influence the adoption and success of robotic cardiovascular surgery. The learning curve for surgeons and teams is substantial, requiring dedicated time for simulation, proctored cases, and progressive case complexity. Docking time, setup logistics, and coordination among anesthesia, perfusion, and nursing teams impact overall operating room efficiency, particularly during the early phases of integration. Tissue handling in a robotic environment relies on indirect feedback, so surgeons must cultivate a nuanced sense of tissue resistance and bleeding patterns through visual cues and instrument behavior, often supplemented by tactile feedback from assistants and careful suction management. The risk of intraoperative complications, such as instrument collisions, air embolism, or inadequate exposure, necessitates rigorous checklists and readiness to convert to a conventional approach if safety margins are compromised. Long operative times in the early learning window can strain resources, underscoring the importance of patient selection and patient-specific risk stratification that balance potential benefits against the procedural demands of robotics. In addition, concerns about cost, instrument wear, and maintenance contribute to a landscape in which robotics is pursued with clear institutional rationale and defined performance targets rather than as an unselective default choice.
Training, credentialing, and team roles
High-quality robotic cardiovascular programs emphasize comprehensive training that combines simulation, anatomy-specific skill acquisition, and mentored clinical cases. Faculty-led curricula typically incorporate staged progression, starting with nonclinical practice, moving through validated simulation modules, and culminating in supervised cases with progressively increasing complexity. Credentialing often depends on demonstrated proficiency in core technical tasks, consistent performance metrics, and positive outcomes across a series of cases. Successful programs cultivate a cohesive team where roles are clearly defined: the surgeon leads the console-based maneuvers, the bedside assistant performs exposure and instrument exchange, the perfusionist manages circulatory support, and the imaging specialist guides intraoperative planning. Regular multidisciplinary debriefings, systematic review of adverse events, and participation in regional or national registries help accelerate collective learning and quality improvement. The emphasis on communication, shared situational awareness, and standardized protocols contributes to safer adoption of robotics in the demanding setting of cardiovascular surgery, where precision and timing can directly impact patient survival and functional recovery.
Economic considerations and health system impact
The financial dimension of adopting robotic systems in cardiovascular surgery involves an intricate balance between capital expenditure, ongoing maintenance, instrument costs, and the potential for workflow efficiencies. Initial investments in robotic platforms are substantial, and hospitals must weigh device depreciation, service contracts, and consumable instrument lifecycles against anticipated throughput, case mix, and payer reimbursement frameworks. While some analyses suggest that shortened hospital stays and reduced blood transfusions may offset portions of the upfront costs, these benefits are highly dependent on case selection, volume, and the efficiency of the surgical program. Institutions also consider opportunity costs, such as the impact on operating room scheduling, staff training time, and the scale of multidisciplinary collaboration required to sustain robotic programs. A thoughtful economic appraisal should accompany clinical planning, including sensitivity analyses for different procedural volumes and long-term maintenance scenarios, to determine whether robotics delivers value within a given health system and patient population.
Patient selection and perioperative planning
Optimal outcomes with robotic cardiovascular surgery begin with careful patient selection. Radiologic and echocardiographic assessment informs decisions about feasibility, anticipated exposure, and technical difficulty, while clinical factors such as comorbidity burden, prior thoracic surgery, and anatomical variations guide suitability. Preoperative planning emphasizes accurate determination of target structures, graft targets, and valve geometry, as well as calibration of anesthetic strategy to accommodate single-lung ventilation, patient positioning, and rapid hemodynamic changes during valve manipulation. In many centers, a multidisciplinary planning conference reviews each candidate case to evaluate potential benefits versus risks, establishing clear expectations for recovery trajectory and informing shared decision making with the patient. Perioperative planning also covers contingency pathways, including criteria for conversion to open surgery and predefined thresholds for anesthesia and perfusion team readiness to ensure patient safety remains paramount throughout the procedure.
Future directions and research
Looking ahead, the trajectory of robotics in cardiovascular surgery is shaped by incremental hardware improvements, software advances, and more robust clinical evidence. Developments aim to enhance haptic or force feedback, enabling a more intuitive sense of tissue interaction that could shorten the learning curve and further reduce tissue trauma. Efforts to miniaturize robotic arms, improve instrument endurance, and expand the repertoire of deliverable procedures will broaden the applicability of robotics to additional cardiac and vascular indications. The integration of artificial intelligence and machine learning may assist with real-time planning, decision support, and quality assurance by analyzing intraoperative imaging and motion patterns to optimize suturing sequences, Prosthesis sizing, and anastomotic geometry. Augmented reality and better imaging fusion could offer enhanced navigation through complex anatomies, while remote collaboration and teleoperation may become more feasible with advances in latency reduction and cybersecurity. As technology evolves, rigorous clinical trials, standardized outcome metrics, and transparent reporting will guide the responsible expansion of robotic capabilities in cardiovascular care, ensuring that innovations translate into meaningful patient benefits and sustainable practice improvements.
Ethical considerations and patient perspectives
Equity of access and informed consent are central ethical considerations in the deployment of robotics in cardiovascular surgery. Patients should receive balanced information about the potential benefits and limitations of robotic approaches relative to conventional methods, including discussions about expected recovery, long-term durability, and the possibility of needing conversion to open surgery. Transparent communication about costs, insurance coverage, and the availability of experienced centers is essential to align patient expectations with feasible options. Ethical deliberations also address disparities in access to advanced technologies, ensuring that the adoption of robotics does not exacerbate existing inequities but rather advances high-quality care for all eligible patients. Patient values, preferences, and goals of care must be integrated into decision making, recognizing that robotic surgery may offer meaningful advantages for some individuals while presenting comparable results for others. This patient-centered approach underscores the principle that technology serves as an enabler of better outcomes, not a substitute for thoughtful clinical judgment and compassionate care.
Safety, quality improvement and regulation
Safeguarding patient safety in robotic cardiovascular surgery relies on rigorous quality improvement frameworks, standardized protocols, and robust data collection. Centers implement safety checklists, participate in surveillance of intraoperative complications, and contribute to national or regional registries that track procedural outcomes, conversion rates, and long-term durability. Regular auditing of operative times, instrument performance, and team communication supports continuous improvement and helps identify opportunities to optimize workflows. Training programs emphasize competency-based milestones, with ongoing mentorship and periodic credentialing reviews to ensure sustained expertise among surgeons and teams. Regulatory and institutional oversight governs device maintenance, sterilization processes, and adherence to best practices, reflecting a patient safety culture that prioritizes meticulous planning, transparent reporting, and rapid response to any adverse events. In this evolving landscape, the ultimate measure of success lies in consistent, patient-centered outcomes that demonstrate meaningful improvements in safety, experience, and quality of life for individuals undergoing cardiovascular procedures with robotic assistance.










