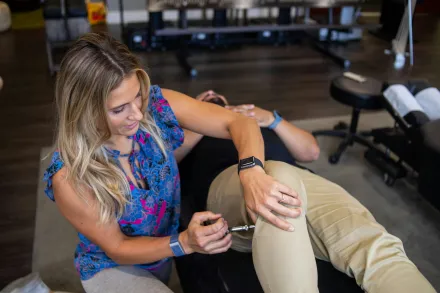
The foundational objectives of physical therapy after stroke
In the wake of a stroke, physical therapy functions as a structured, patient centered pathway designed to reduce disabling consequences and restore meaningful movement. Therapists begin by appreciating the unique pattern of weaknesses, spasticity, sensory changes, and cognitive demands each person faces, recognizing that recovery unfolds along multiple domains rather than a single metric. The core objectives are to limit secondary complications such as contractures, pressure injuries, and deconditioning, to promote safe mobility and independence in daily life, and to align therapeutic activities with what the person values most, such as walking to a loved one's home, preparing meals, or managing medications. By combining careful assessment with evidence informed interventions, physical therapy creates a scaffold for progress that respects the pace of the brain’s adaptation while providing clear, achievable milestones. This approach is guided by a holistic view of health that encompasses physical capacity, emotional well being, and social participation, and it emphasizes collaboration with families and caregivers to sustain gains beyond the clinic walls.
Understanding neuroplasticity and motor recovery
Neuroplasticity is the central mechanism by which recovery occurs after stroke, and physical therapy is designed to harness repetitive, meaningful movement to shape neural networks. The brain rewires itself through practice that is task specific, progressively challenging, and embedded in real life situations. When a patient attempts a movement, the nervous system interprets errors and recalibrates motor commands, strengthening pathways that enable smoother, more coordinated action. This learning process relies on well calibrated sensory feedback, attention, motivation, and adequate arousal, all of which therapists support through careful task selection and pacing. Importantly, recovery is heterogeneous; some functions improve quickly while others require persistent practice over weeks and months. The therapist structures sessions to optimize neuroplastic changes while avoiding fatigue and frustration that can dampen learning.
Initial assessment and goal setting
Initial assessment in physical therapy for stroke involves mapping the strengths and limitations of the affected limb, evaluating sensation, range of motion, coordination, balance, gait, and endurance, and observing how cognitive factors influence movement. A collaborative goal setting process brings the patient and family into the plan, translating clinical findings into meaningful everyday activities. Goals are described in measurable terms but also framed within a timeline that remains flexible as adaptation occurs. The therapist uses standardized measures when appropriate but mostly relies on real world observations to understand how impairments shape participation. This early alignment creates a shared vision that guides therapy through the next weeks and helps families anticipate the pace and scope of progress.
Early mobilization and safe positioning
Early mobilization and safe positioning are critical for preventing complications and maintaining joint and muscle health during the acute and subacute phases. Therapists teach bed mobility, rolling, sitting tolerance, and transitional movements with attention to safety cues, transfer techniques, and the use of assistive devices where indicated. Positioning strategies reduce the risk of contractures and pressure injuries while promoting proprioceptive input that helps the nervous system recalibrate postural control. Even in the most challenged cases, gentle, purposeful movement is pursued to activate circuits without provoking pain or overwhelming the patient, gradually building endurance and confidence. This phase also emphasizes communication, so patients can express discomfort, fatigue, or goals even when speech or cognition is temporarily affected.
Gait reeducation and balance training
Gait reeducation and balance training focus on restoring the ability to move safely across different surfaces and environments, with an emphasis on symmetry, efficiency, and endurance. Therapists analyze walking patterns using observation, cues, and sometimes simple measurement tools to identify compensations that may burden joints or limit function. Interventions include task specific practice such as overground walking, treadmill training, and obstacle negotiation, complemented by strengthening, flexibility, and sensory re–education for the legs and trunk. Balance training enhances postural control through progressive challenges, such as dynamic weight shifts, perturbations, and dual task practice that simulates real life demands. The goal is not only speed but also stability and confidence in navigating stairs, curbs, and uneven ground.
Upper limb recovery strategies
Upper limb recovery is often one of the most stubborn challenges after stroke, yet it is essential for independence in daily tasks and for the emotional well being of the person. Physical therapy uses a combination of task oriented practice, proprioceptive stimulation, and strength training to promote finger and hand function, grasp, release, and fine motor control. Therapists select activities that mimic daily tasks such as reaching for objects, manipulating utensils, or dressing, ensuring that movements are meaningful and motivating. Techniques may include repetitive practice of isolated movements to rebuild motor patterns and functional integration, with careful attention to spasticity and coordination. By pairing motor relearning with sensory feedback, therapists help the affected limb regain a more natural sense of control and a sense of ownership over everyday activities.
Constraint-induced movement therapy and task-specific practice
Constraint induced movement therapy and task specific practice are powerful approaches for encouraging use of the affected limb, especially when voluntary use is limited. In this approach, the unimpaired limb is restrained in a safe way to compel reliance on the affected side, while practice sessions target functional tasks. The underlying principle is that the brain learns most effectively when a person must solve problems with the impaired limb, thereby driving cortical reorganization and improving dexterity. Ethical and practical considerations are important, including ensuring the patient’s comfort, monitoring for fatigue, and tailoring the intensity to avoid frustration. When applied judiciously within a broad rehabilitation plan, constraint induced therapy can yield meaningful improvements in reach, grip, and coordination that translate into daily living activities.
Mirror therapy and mental imagery
Mirror therapy and mental imagery provide creative avenues for activating motor circuits even when movement is limited. In mirror therapy, the patient observes a reflection of the unaffected limb performing tasks while the affected limb remains still, creating a visual illusion that promotes motor planning and reduces phantom sensations of paralysis. Mental imagery involves imagining the execution of movements without actual muscle activation, engaging similar neural networks that support real movement. Both approaches are integrated with conventional therapy to reinforce learning, improve attention to the affected side, and gradually expand voluntary control. The effectiveness of these strategies is enhanced when combined with real task practice and patient engagement, reinforcing the idea that perception and intention can shape physical outcomes.
Strengthening and resistance training
Strengthening and resistance training form a core component of post stroke rehabilitation, addressing muscle weakness that undercuts balance, gait, and daily function. Therapists design progressive programs that begin with low resistance and high reps, then carefully scale intensity based on the patient’s response, fatigue levels, and joint safety. Emphasis is placed on functional movements that mirror daily tasks, such as standing from a chair, transferring, lifting objects, and stabilizing the trunk during reaching. In addition to traditional weights, resistance bands and gravity assisted tools are used to modulate effort while protecting joints. The gains extend beyond the muscles themselves, contributing to improved motor planning, confidence, and participation in life roles.
Endurance and aerobic conditioning
Endurance and aerobic conditioning play a vital role in overall health and stroke recovery, supporting cardiovascular function, energy reserves, and mood. Physical therapists tailor aerobic programs to the individual's history and current fitness level, gradually increasing walking time, cycling, swimming, or other rhythmic activities as tolerated. It is important to monitor heart rate, blood pressure, and perceived exertion to maintain safe levels of exertion while avoiding fatigue that could trigger confusion or a fall. Regular aerobic training improves cerebral perfusion and metabolic efficiency, which may facilitate learning and recovery. In addition, conditioning positively affects sleep, appetite, and motivation, all of which are integral to sustaining a long term rehabilitation plan.
Postural control and trunk stability
Postural control and trunk stability are foundational for coordinated movement, balance, and safe function in upright activities. Therapists assess how the spine, pelvis, and shoulder girdle contribute to posture and how compensations in one area affect another. Interventions emphasize core activation, spinal alignment, and controlled transitions between positions. Exercises might include seated and standing balance tasks, progressive rotational movements, and trunk stabilization exercises that are integrated with limb movements to promote efficient, coordinated patterns. Improved trunk control reduces fall risk and underpins the ability to perform complex tasks such as reaching, bending, and stepping. The emphasis is on maintaining proper alignment while allowing adaptive strategies that support independence in daily life.
Functional task practice
Functional task practice anchors rehabilitation in the realities of daily living, ensuring that improvements in strength, sensation, and motor control translate into practical capabilities. Therapists select activities that reflect the patient’s routine, preferences, and environmental constraints, then recreate those tasks in a controlled setting with safety and feedback. Repetition, error based learning, and graded challenges help the nervous system refine movement strategies, timing, and coordination. The practice extends across the day, with attention to different contexts such as home, work, community, and transportation. By repeatedly solving real problems, patients develop confidence and autonomy, reducing reliance on caregivers and enhancing life satisfaction.
Assistive devices and adaptive equipment
Assistive devices and adaptive equipment support safety and independence when certain movements are not yet feasible. Physical therapists assess the need for canes, walkers, orthoses, braces, or footwear modifications, and help patients learn to use these tools effectively so they complement therapy rather than hinder progress. The selection process considers the individual’s goals, environment, and comfort level, as well as potential long term benefits such as improved posture, reduced energy expenditure, and enhanced mobility. Proper fitting, instruction, and progressive training ensure users gain confidence and competence, enabling them to pursue activities that matter most without fear of falls or instability.
Home exercise programs and caregiver involvement
Home exercise programs and caregiver involvement are essential to sustaining gains after leaving the clinical setting. Therapists collaborate with patients and families to design practical routines that fit daily schedules, living spaces, and transportation options, ensuring exercises are safe, varied, and aligned with long term goals. Clear written instructions, demonstrations, and periodic follow up visits or telehealth check ins support adherence and adjust plans as recovery unfolds. Caregivers play a vital role in providing encouragement, monitoring fatigue, and facilitating accessibility. The aim is to create an empowering, shared responsibility so that progress continues beyond formal therapy sessions and becomes a living practice embedded in everyday life.
Safety, risk management, and education
Safety, risk management, and education underpin every phase of physical therapy after stroke. Therapists educate patients and families about recognizing warning signs of complications, managing fatigue, and pacing activities to avoid setbacks. They assess home environments for hazards, teach transfer and wheelchair safety, and develop fall prevention strategies that are realistic and feasible. Education includes information about medication interactions, energy conservation, adaptive strategies for communication, and the use of assistive devices so that patients can participate safely in community life. By embedding safety into routine practice, therapists empower patients to take calculated risks, push boundaries where appropriate, and maintain progress without compromising well being.
Interdisciplinary collaboration and continuity of care
Interdisciplinary collaboration and continuity of care are essential to comprehensive stroke rehabilitation, integrating physical therapy with occupational therapy, speech language pathology, neuropsychology, medicine, and social work. A cohesive team coordinates assessment, goal setting, and progression, ensuring that interventions in one domain support improvements in others. Regular communication among clinicians, patients, and families helps align expectations, monitor complications, and adapt plans as cognitive, emotional, or medical changes occur. The continuity of care extends into outpatient, community based, and home settings, with therapists advocating for timely access to resources, transportation, and social supports. This collaborative approach amplifies recovery, opening pathways to independence that persist long after discharge from acute care and inpatient rehabilitation.










