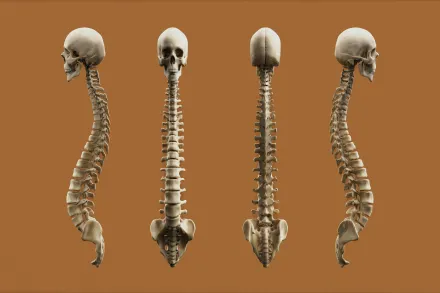
Understanding Osteoporosis
Osteoporosis is a chronic condition of the bones that emerges when the balance between bone building and bone loss shifts toward net loss, resulting in porous, fragile skeletal tissue with reduced strength. This disorder is not simply a matter of aging but a complex interplay of genetic factors, hormonal influences, environmental exposures, nutrition, physical activity, and comorbid illnesses that can accelerate bone deterioration. When bone density declines and the microarchitecture of bone becomes compromised, a minor fall or even a sudden twist can produce a fracture that carries significant consequences for mobility, independence, pain, and overall health. The spine, hip, and forearm are among the most vulnerable sites, yet fractures can occur at other locations as bone quality wanes. Understanding osteoporosis requires recognizing that bone remodeling is a lifelong process in which old bone is resorbed by cells called osteoclasts and new bone is laid down by osteoblasts, and that aging, hormonal changes, and lifestyle choices can alter the rate of this remodeling in ways that favor fragility. Long before a fracture happens, subtle signs may exist in bone density measurements and in markers of bone turnover, and recognizing these signs allows for early intervention that can slow or even partially reverse the trajectory of bone loss. In addition, the experience of a fragility fracture itself signals the need to reassess risk factors, adherence to treatment, and strategies for preventing future injuries, because the risk of subsequent fractures typically remains elevated for years after the first event. The overarching aim of prevention and management is to preserve bone strength, reduce fracture risk, improve physical function, and maintain quality of life through a combination of practical lifestyle choices, targeted medical therapies when indicated, and ongoing monitoring. The path for each individual is shaped by personal priorities, medical history, and the potential benefits and risks of interventions, all of which should be discussed in a collaborative relationship with health care professionals who specialize in bone health.
In practical terms osteoporosis reflects a loss of skeletal resilience rather than a single symptom, and its impact extends beyond the bones themselves. Fragility fractures can lead to chronic pain, limited mobility, extended hospital stays, and a cascade of complications such as fear of falling, social isolation, and dependence on others for daily activities. The effort to prevent these outcomes thus encompasses a broad view of health that includes cardiovascular risk management, metabolic balance, muscle strength, balance and coordination, and the social determinants of health that influence access to nutrition, exercise opportunities, and medications. A successful approach is proactive rather than reactive, prioritizing bone health as a lifelong aspect of wellness rather than a problem discovered only after a fracture. The interplay between bone density, bone quality, and fracture risk means that clinicians consider multiple dimensions when assessing risk and tailoring treatment to individual needs. This holistic view supports not only physical resilience but also emotional and social well being as people age.
Advances in diagnostic technologies and a growing understanding of the biology of bone remodeling have refined how osteoporosis is identified and treated. While bone mineral density measurements provide a quantitative picture of bone mass, they do not capture every facet of fracture risk. Combining imaging with clinical risk factors such as age, sex, family history, prior fractures, and lifestyle factors creates a more complete assessment. Consequently, prevention strategies emphasize a continuum that begins early, continues through adulthood, and intensifies as risk rises. This continuum includes surveillance of nutritional status, physical activity patterns, metabolic conditions, and medications that influence bone metabolism, along with patient engagement in adopting sustainable habits that protect bone health over time. The overall goal is to maintain bones that can withstand everyday stresses while preserving the ability to move freely and pursue activities that matter to each person.
Risk Factors and Screening Guidelines
Risk factors for osteoporosis are both modifiable and nonmodifiable, and understanding them helps individuals and clinicians identify those who may benefit most from preventive measures. Nonmodifiable factors include advancing age, female sex especially after menopause, a family history of osteoporosis or fractures, and certain genetic conditions that influence bone metabolism. Hormonal changes that accompany menopause, prolonged exposure to low estrogen levels, and particular endocrine disorders can accelerate bone loss, particularly in women, though men also experience bone thinning with age. Body size, prior fractures, and certain chronic diseases such as rheumatoid arthritis, inflammatory bowel disease, and chronic kidney disease contribute to an elevated fracture risk. Lifestyle elements that escalate risk include inadequate calcium or vitamin D intake, a sedentary lifestyle, excessive alcohol consumption, smoking, and prolonged use of certain medications that interfere with bone turnover, such as corticosteroids. Understanding the intersection of these factors helps guide conversations about screening and prevention.
Screening for osteoporosis typically involves evaluating bone density using a measure known as dual-energy X-ray absorptiometry, or DXA, which yields a numerical score reflecting bone mineral density and allows comparison to a young healthy reference population. In addition to imaging, clinicians may assess clinical risk using tools that weigh factors such as age, height loss, a prior fracture after minimal trauma, smoking status, and other health conditions that influence bone strength. The screening approach is tailored to an individual’s age, sex, medical history, and risk factors. For many adults, initial bone density testing is recommended around the time of menopause for women and at an older age for men, with intervals for repeating testing determined by results and evolving risk. In younger adults with secondary causes of bone loss or with ongoing risk factors, clinicians may initiate evaluation earlier and monitor more closely. Regular monitoring supports timely adjustments to lifestyle and treatment plans so that fracture risk can be kept as low as possible over time.
The implications of fracture risk extend beyond the bones themselves, affecting independence and daily functioning. Therefore, screening protocols emphasize not only measuring bone density but also integrating information about falls risk, gait stability, vision, medication effects, and home environment. A comprehensive approach to screening considers the likelihood that an individual will benefit from preventive actions, including lifestyle modifications and pharmacologic therapy when warranted. When screening identifies lower bone mass or higher fracture risk, clinicians can discuss the spectrum of preventive measures, balancing efficacy, safety, tolerability, and patient preferences to arrive at a plan that is realistic and sustainable. The goal of this process is to empower individuals with knowledge about their bone health and to translate that knowledge into concrete steps that lower the chance of fractures while supporting overall health.
From a public health perspective, recognizing high-risk populations and ensuring access to screening are essential components of reducing fracture burden. Age, sex, and comorbidity patterns vary across communities, and so do dietary patterns and opportunities for physical activity. Efforts to improve screening uptake benefit from clear communication about the benefits of early detection, the safety and convenience of testing, and the potential impact of preventive strategies on long-term health outcomes. For clinicians, a patient-centered approach that respects values and preferences, while presenting evidence-based recommendations, fosters trust and engagement in preventive care. In this way, risk assessment becomes a collaborative process that informs lifestyle choices, environmental modifications, and medical decisions designed to preserve bone health across the lifespan.
Nutrition, Calcium, Vitamin D, and Other Nutrients
Nutrition provides the foundation for bone health, supplying the building blocks and environmental context for healthy remodeling. Adequate calcium intake supports the mineral reservoir in bone, while vitamin D enhances calcium absorption and bone mineralization. A balanced diet that includes dairy products, fortified foods, leafy greens, and fish provides calcium in combination with other nutrients that support skeletal integrity. The interplay between calcium and vitamin D is particularly important because insufficient vitamin D reduces calcium absorption and can contribute to secondary bone loss, especially in older adults who may have reduced sun exposure and limited dietary intake. Ensuring sufficient vitamin D through sun exposure, fortified foods, or supplementation is a practical component of prevention strategies, with individualized targets guided by health status and laboratory measurements when appropriate.
Beyond calcium and vitamin D, other nutrients contribute to bone strength and muscle function, which in turn influence fall risk and fracture potential. Protein intake supports muscle mass, a key factor in maintaining stability and preventing frailty. Magnesium and phosphorus participate in bone mineralization and energy metabolism, while micronutrients such as zinc, boron, and vitamin K play roles in collagen formation and bone turnover, though the specific supplementation needs may vary among individuals. A well-rounded diet emphasizes fruits, vegetables, whole grains, and lean sources of protein, along with limited processed foods and added sugars, creating an overall metabolic environment that promotes bone health. Adequate hydration and a careful approach to caffeine and sodium intake can also influence bone metabolism and calcium balance, reinforcing the idea that dietary patterns as a whole contribute to skeletal resilience.
In some cases nutrition alone cannot fully prevent bone loss, particularly when other risk factors are present or when malabsorption or chronic disease limits nutrient status. In those situations clinicians may recommend targeted supplementation with calcium and vitamin D at prescribed doses, and they may monitor blood levels and urinary excretion markers to adjust therapy accordingly. The goal is not simply to reach a given numeric target but to support sustained bone health in the context of a person’s overall health profile, medications, and daily life. Education about reading labels, recognizing fortified foods, and planning balanced meals can empower individuals to maintain nutritional habits that support bone integrity over years and decades.
Exercise and Physical Activity for Bone Health
Physical activity stands as a central pillar of osteoporosis prevention and management because bones respond to mechanical loading with adaptive remodeling. Weight-bearing activities, such as walking, hiking, stair climbing, or dancing, stimulate bone formation in weight-bearing bones and help preserve density as well as bone geometry. Resistance training, using free weights, machines, or resistance bands, fosters muscle strength and improves the forces that bones experience during daily activities, contributing to fracture resistance. Balance and coordination exercises, including tai chi or specific balance routines, reduce the likelihood of falls by enhancing proprioception and postural stability, which is particularly valuable for older adults who face a higher risk of accidental injuries. The combined effect of these modalities supports both skeletal health and functional independence, enabling individuals to maintain activity levels that contribute to overall well-being.
Engaging in an exercise program with professional guidance can tailor intensity and progression to an individual’s baseline fitness, bone health status, and comorbidities. A gradual approach that respects joint health and cardiovascular capacity minimizes the risk of injury while maximizing benefits. For many people, a routine that blends aerobic activity, resistance training, and balance work provides the most effective protection against fractures. Incorporating activities into daily life, such as taking stairs instead of escalators when feasible, performing light resistance exercises at home, and cultivating a habit of regular movement, reinforces the long-term value of physical activity for bone health. The emphasis remains on consistency, safety, and personalization rather than on intense or unsustainable regimes.
In addition to structured exercise, posture training, core stabilization, and flexibility work support healthy spinal alignment and reduce the likelihood that vertebral fractures will produce pain or deformity. Clinicians often collaborate with physical therapists to design exercise plans that accommodate any existing musculoskeletal conditions and to monitor tolerance, progression, and response to therapy. When barriers arise such as pain, fatigue, or fear of falling, addressing these concerns with a multidisciplinary team helps maintain participation and prevents gaps in care that could undermine bone health over time. The overarching message is that movement matters, and that a thoughtful, supervised program can yield meaningful gains in bone strength and functional capacity.
Medications for Osteoporosis
Medications used to prevent fractures and preserve bone strength target different aspects of bone remodeling, and the choice among them depends on an individual’s risk profile, tolerability, and medical history. Antiresorptive agents slow bone loss by reducing the activity of osteoclasts, thereby helping to maintain existing bone structure and density. These therapies include bisphosphonates, which can be taken orally or by infusion, and denosumab, a monoclonal antibody administered by injection that decreases bone resorption. For some individuals with severe osteoporosis or very high fracture risk, anabolic agents stimulate bone formation by osteoblasts and may be used to build new bone, with careful consideration of duration and monitoring requirements. Among older options, selective estrogen receptor modulators provide estrogen-like effects in bone tissue, offering another mechanism to preserve bone density in appropriate patients. The decision framework for medication considers efficacy, potential side effects, adherence considerations, renal function, and the presence of other medical conditions that might influence safety. In the context of comprehensive care, pharmacologic therapy is often paired with lifestyle modifications, nutrition optimization, and fall prevention strategies to amplify protection against fractures.
Adherence to prescribed medications is a critical determinant of success in osteoporosis management. Some treatments require regular administration over years, and missed doses or irregular follow-up can diminish benefits. Patients may encounter side effects such as gastrointestinal symptoms with some oral bisphosphonates or transient hypocalcemia with certain agents, and clinicians work with individuals to manage these issues through timing, formulation choice, or alternative therapies. Shared decision-making that respects patient preferences, concerns, and daily routines supports sustained adherence and better outcomes. In clinical practice, periodic reassessment of fracture risk, bone density, and functional status informs adjustments in therapy, including changes in medication or the introduction of supplementary strategies to optimize bone health. The ultimate aim is to reduce fracture incidence while maintaining overall safety and quality of life.
Fall Prevention and Home Safety
Preventing falls is a practical, essential aspect of protecting bones, especially in older adults or individuals with impaired balance or gait. Environmental modifications in the home, such as installing secure lighting, removing tripping hazards, adding grab bars in bathrooms, and ensuring stable footwear, can substantially reduce the risk of injury. Regular vision checks and managing medications that affect alertness or balance are important complementary steps. Engaging in balance and strength training, as discussed in the exercise section, complements environmental changes by enhancing the body’s ability to react quickly to destabilizing situations. A personalized plan often includes a review of daily routines, assistive devices when needed, and education about how to fall safely when avoidance is not possible. The goal is to minimize the chance of a fracture from a fall while maintaining independence and confidence in daily activities.
Addressing fall risk involves considering bone health in the broader context of aging and chronic disease management. Chronic conditions such as arthritis, neuropathy, or cognitive impairment can contribute to parallel challenges that raise the probability of a fall. A multidisciplinary approach that includes physical therapy, occupational therapy, and primary care coordination helps to identify and mitigate these risks. Practical strategies extend beyond the home to community environments, where safe walking paths, accessible transportation, and social support networks can encourage continued physical activity, which in turn supports both bone and muscle health. By combining protective home design with proactive movement and medical optimization, the likelihood of falls leading to fractures can be meaningfully reduced.
Education plays a pivotal role in fall prevention. Patients and caregivers benefit from clear information about the signs of balance decline, safe techniques for transfers and transfers in and out of chairs or beds, and the importance of reporting new dizziness, headaches, or visual changes promptly. Clinicians can provide resources that help individuals apply these principles in daily life, reinforcing a culture of safety and resilience. When fall risks are significant, arranging community-based programs and home health support can supplement the clinical plan, ensuring that safe environments and supportive routines are accessible. The combined effect of environmental adjustments and proactive movement strategies contributes to a meaningful reduction in fracture risk and an enhanced sense of security.
Special Considerations Across Populations
Osteoporosis affects individuals differently depending on age, sex, hormonal status, and comorbidity patterns. In postmenopausal women, the rapid decline in estrogen accelerates bone loss, making prevention and early intervention particularly important after menopause. In men, osteoporosis is less common but often underrecognized, and risk increases with age and comorbid conditions such as gonadal dysfunction or medications that influence bone turnover. In younger people, secondary bone loss can arise from endocrine disorders, renal disease, inflammatory conditions, or certain medications, and identifying these drivers is essential to interrupting progression. Across age groups, physical activity, nutrition, and appropriate medical therapy play key roles in maintaining bone health, but the balance between benefits and risks of pharmacologic treatment may differ. For older adults with multiple health issues, treatment decisions require careful consideration of competing priorities, overall goals, and the potential impact on daily functioning. In all populations, patient education about bone health, treatment options, and practical strategies fosters autonomy and informs choices aligned with personal values.
The social and economic context also shapes osteoporosis management. Access to screening, the availability of osteoporosis specialists, affordability of medications, and the capacity to implement exercise programs all influence outcomes. Efforts to reduce disparities involve public health initiatives that promote awareness, expand coverage for testing and medications, and provide community resources for safe physical activity and nutrition. The patient journey is not limited to a single medical encounter but extends into daily life, where ongoing support, reminders, and coaching can sustain adherence and motivate continued engagement in bone health. In this broader view, prevention and management become collective efforts that bring together clinicians, patients, families, and communities to preserve mobility, independence, and vitality over time.
Monitoring Bone Health and Treatment Efficacy
Ongoing monitoring ensures that preventive and therapeutic strategies remain appropriate as health status evolves. Regular assessment of bone density through DXA, when indicated, provides a quantitative gauge of response to therapy, while clinical evaluation tracks fracture history, functional capacity, and tolerability of treatments. Laboratory tests may be used to monitor vitamin D status, calcium balance, kidney function, and markers of bone turnover in certain scenarios, helping clinicians tailor interventions to current needs. Periodic re-evaluation of risk factors, nutritional status, and activity levels supports dynamic adjustments to lifestyle plans and medications. The aim is not only to slow bone loss but to prompt timely changes that maintain or enhance bone strength and reduce fracture incidence over time. This adaptive approach recognizes that health is a moving target and that proactive reassessment is essential to sustaining gains achieved through prevention and treatment.
By maintaining open communication about symptoms such as new back pain, height loss, or changes in posture, individuals can contribute to early detection of vertebral fractures or other skeletal concerns. Clinicians use these signals to determine whether imaging, laboratory work, or therapy modifications are warranted. The monitoring process also includes evaluating adherence and tolerability, because real-world effectiveness depends on how patients integrate recommendations into daily life. A transparent, collaborative dialogue about goals, progress, and challenges supports a sustainable plan that remains aligned with personal priorities and medical realities. In this way, monitoring becomes a cornerstone of long-term bone health that adapts as circumstances change and as new evidence informs best practices.
Emerging Therapies and Research
Research in osteoporosis continues to expand the range of options for prevention and treatment, with innovations aimed at improving efficacy, safety, and convenience. New therapeutic targets seek to influence the complex signaling pathways that regulate bone formation and resorption, potentially offering benefits for individuals who respond poorly to existing therapies or who experience intolerable side effects. Advances in personalized medicine hold promise for tailoring interventions to a person’s genetic profile, lifestyle, and comorbidity landscape, improving the precision of risk stratification and the selection of the most suitable agents. In parallel, studies explore optimal durations of therapy, strategies for drug holidays where appropriate, and combinations that maximize bone density gains while minimizing adverse effects. Ongoing investigations into the biology of aging, muscle-bone crosstalk, and the interplay between nutrition and pharmacology continue to inform clinical practice and public health policy. This evolving landscape invites clinicians and patients to engage in informed discussions about emerging options and to participate in research opportunities when appropriate, contributing to collective progress in reducing fracture risk and enhancing quality of life.
Technological developments, such as improved imaging techniques and digital health tools, are enhancing how bone health information is collected, interpreted, and acted upon. Telemedicine capabilities facilitate regular follow-up, particularly for individuals living in areas with limited access to specialized care. Digital platforms can support adherence, symptom tracking, and remote coaching for exercise programs, helping to bridge gaps that previously limited the reach of preventive strategies. While these innovations hold considerable promise, they also require careful attention to data privacy, equitable access, and validation in diverse populations. The goal remains clear: translate scientific advances into practical, patient-centered care that reduces fractures, preserves mobility, and supports a high quality of life across the lifespan.
Empowering Patients through Education and Access
Education is a powerful tool that enables people to take control of their bone health and to engage thoughtfully with health care teams. Clear explanations of risk factors, test results, and treatment choices help individuals make informed decisions that align with their values and lifestyles. Educational efforts extend to practical skills such as how to read nutrition labels, plan meals that meet calcium and vitamin D needs, understand medication instructions, and identify safe and enjoyable forms of physical activity. Access to reliable information reduces confusion, supports adherence, and fosters a sense of partnership between patients and clinicians. Equally important is ensuring access to screenings, diagnostic services, medications, and rehabilitation resources, so that preventive measures are available to diverse communities. By removing barriers and building supportive networks, health systems can help more people benefit from evidence-based strategies that strengthen bone health.
Incorporating preventive care into routine health maintenance conversations encourages a proactive mindset, where individuals are encouraged to attend regular checkups, discuss changes in health or mobility promptly, and pursue appropriate tests when indicated. This approach recognizes that osteoporosis is a long-term condition that benefits from consistent attention rather than episodic interventions. Emphasis on shared decision-making, respect for patient preferences, and attention to cultural and socioeconomic factors helps ensure that prevention and management strategies are realistic, acceptable, and sustainable for each person. The cumulative effect of education, accessibility, and ongoing support is a healthier population with fewer fractures, preserved independence, and enhanced well-being.