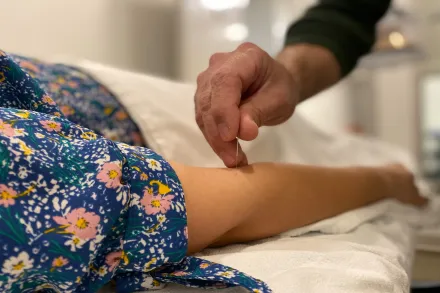
Across centuries and continents, acupuncture has evolved from its traditional roots in East Asian medicine into a widely recognized approach for addressing pain in modern clinical settings. The practice rests on a combination of historical observation and contemporary clinical inquiry, weaving together ideas about energy flow, known as qi in traditional theories, with modern concepts of nervous system signaling and biochemical responses. Patients seeking relief from persistent discomfort often report a sense of release that extends beyond the moment of needle insertion, and clinicians frequently observe improvements in mobility, sleep, and overall well-being as pain signals diminish. This article explores how acupuncture may relieve pain, what kinds of pain most commonly respond, how evidence supports these claims, what a typical session looks like, safety considerations, and how acupuncture fits into a broader strategy of care. The discussion emphasizes patient-centered care, the complexity of pain as an experience that involves sensation, emotion, cognition, and context, and the idea that acupuncture can be a meaningful component of an integrative approach rather than a solitary solution.
Historical roots and evolving practice
Acupuncture emerged from a long-standing tradition in which practitioners sought to rebalance bodily energies through precise stimulation of specific points along pathways known as channels or meridians. Over time, this framework began to converge with scientific inquiry as researchers began to map physiological responses to needle insertion using modern instruments and methodologies. In contemporary practice, licensed acupuncturists combine traditional diagnostic observations with patient history, lifestyle assessment, and a careful physical examination to develop individualized treatment plans. The act of inserting fine sterile needles at defined locations is paired with careful technique, depth, and duration, often accompanied by a gentle, relaxing environment and breathing guidance that helps patients become more attuned to bodily sensations. The result is a patient experience that blends ritual, clinical skill, and measurable change in the nervous system’s processing of pain signals. As the practice has broadened, practitioners have integrated ultrasound guidance, evidence-informed point selection, and standardized safety procedures while maintaining respect for the patient’s subjective experience of relief and comfort.
How acupuncture may relieve pain
Many researchers propose that acupuncture influences pain relief through several interacting mechanisms. At the neurochemical level, stimulating specific points can trigger the release of endorphins and endogenous opioid peptides, which modulate pain perception and contribute to a sense of well-being. At the neural circuitry level, acupuncture is thought to activate afferent nerve fibers that engage brain circuits involved in pain modulation, mood regulation, and autonomic balance. This activation can alter the way pain signals are processed in the spinal cord and brain, increasing the threshold for pain and reducing the intensity of discomfort experienced. Additionally, acupuncture may exert anti-inflammatory effects by influencing immune signaling pathways, which can be relevant in conditions where inflammatory processes contribute to pain. Beyond these physiological changes, patients often report improvements in sleep, mood, and stress resilience following treatment, which can create a positive feedback loop that enhances overall pain management. It is important to recognize that the experience of pain is multifaceted, and placebo effects, patient expectations, and the therapeutic context can contribute to perceived benefit. The combination of physiological mechanisms with contextual factors can yield meaningful, real-world improvements for individuals dealing with chronic or acute pain.
Types of pain commonly addressed
Acupuncture is frequently sought for musculoskeletal pain, including back and neck pain, shoulder stiffness, and knee discomfort from degenerative changes or overuse. It is also used for headaches and migraines, where neural pathways, vascular dynamics, and inflammatory mediators can all contribute to the attack or baseline vulnerability. Neuropathic pain arising from nerve injury or conditions such as postherpetic neuralgia can respond to acupuncture through modulation of somatosensory processing and reduced nerve sensitization. In addition, some patients with fibromyalgia or generalized widespread pain report improvements in pain intensity and fatigue, though outcomes can vary and are influenced by the presence of sleep disturbances, mood symptoms, and comorbid conditions. The breadth of conditions where acupuncture appears beneficial reflects its potential to influence multiple systems involved in pain—peripheral tissues, the central nervous system, and the psychophysiological state of the individual—while remaining most effective in pain syndromes with clear musculoskeletal or inflammatory components.
Evidence from research
Clinical research on acupuncture has grown substantially, with systematic reviews and meta-analyses offering nuanced conclusions. Across several common pain conditions, including low back pain, osteoarthritis, and tension-type headaches, randomized trials and comparative studies have shown that acupuncture can produce small to moderate improvements in pain and function, often surpassing those seen with sham procedures in some analyses. The magnitude of benefit varies across studies, and heterogeneity in study design, patient expectations, and practitioner technique can influence results. Importantly, many reviews emphasize that acupuncture is generally safe when performed by trained professionals using sterile equipment, with adverse events typically limited to transient soreness, minor bruising, or fatigue. The growing body of evidence supports acupuncture as a viable option within an interdisciplinary approach to pain that also includes physical therapy, exercise, psychosocial support, and conventional medical treatments when warranted. For patients who respond to it, acupuncture can provide meaningful relief that reduces reliance on medications and contributes to improved daily functioning.
What to expect in an acupuncture session
A typical session begins with a warm, welcoming assessment in which the practitioner listens to the patient’s description of pain, daily activities, and goals for treatment. The subsequent plan may involve selecting a cluster of points that address the location and character of the pain, as well as related areas that influence the body’s regulatory systems. The actual insertion of hair-thin needles is often painless or accompanied by a mild pricking sensation as the needle reaches the correct depth. Patients frequently experience a sense of relaxation known as calmness or a deep sensation that is described as de qi by some practitioners. The needles are usually left in place for a short period, during which time breathing guidance, music, or a quiet environment may help the patient relax further. After removal, the practitioner may discuss self-care strategies, such as gentle stretching, hydration, and activity pacing, to support ongoing benefits. A course of treatment often involves multiple sessions over several weeks, with adjustments to the plan based on the patient’s response, changes in pain intensity, and evolving functional goals.
Safety, safety concerns, and who should avoid acupuncture
Acupuncture is considered safe when performed by trained and licensed professionals who adhere to strict hygienic standards and single-use needles. The risk profile is generally low and includes minor transient effects such as soreness at needle sites, lightheadedness, or temporary fatigue. More serious risks, such as infection or injury, are uncommon when proper protocol is followed. People with certain medical conditions or circumstances should discuss acupuncture with their healthcare providers before starting treatment. For instance, individuals with bleeding disorders or who use anticoagulant medications may require special precautions. Pregnant individuals should seek guidance from their providers about acupuncture, as certain points are traditionally avoided or used with caution during pregnancy. Practitioners typically screen for these considerations during an initial intake and tailor the plan to minimize risk while maximizing benefit. Overall, safety hinges on the practitioner’s training, adherence to sterile technique, and clear communication about any health concerns.
Interplay with conventional medicine and self-care
Acupuncture works best as part of a broader, integrative strategy rather than as a sole remedy for complex pain conditions. In many cases, conventional medical evaluations, imaging when indicated, physical therapy, and appropriate medications form a framework within which acupuncture can be added to address symptoms and improve function. The passive act of receiving acupuncture can be complemented by active self-care practices such as guided breathing, mindfulness, safe stretching routines, posture optimization, and gradual progression of physical activity. When clinicians coordinate care, patients often notice improvements in sleep quality, mood, and daytime energy, all of which contribute to a more resilient response to pain. A key advantage of integrating acupuncture is the potential to reduce dependence on analgesics, including nonsteroidal anti-inflammatory drugs and, when appropriate, opioid medications, while still maintaining effective symptom control. This collaborative approach respects patient preferences and emphasizes personalized treatment plans that consider the whole person, not just the pain.
Choosing a practitioner and setting expectations
Selecting a qualified practitioner is a central step in achieving safe and meaningful benefits from acupuncture. Potential patients may seek recommendations from trusted healthcare providers, friends, or local professional directories, and they should verify licensure, certification, and adherence to established safety standards. A good practitioner will conduct a thorough intake, explain the rationale for chosen points, discuss the expected pace of improvement, and address any concerns about side effects or interactions with other treatments. Realistic expectations matter; acupuncture tends to reduce pain intensity and improve function gradually, often in combination with other therapies, rather than delivering dramatic, immediate cures. Many patients report a sense of overall wellness and stress relief that complements improvements in pain, which can enhance motivation to maintain a regular treatment schedule and engage in supportive activities such as gentle exercise, nutrition, and sleep hygiene.
Acupuncture in special populations
People with chronic illnesses, older adults, athletes, and individuals seeking non-pharmacological pain relief can benefit from acupuncture, but special considerations apply. In athletes, acupuncture may support recovery, reduce muscle tension, and facilitate training continuity by alleviating fatigue-related pain and stiffness. For older adults, individualized treatment plans consider coexisting conditions, age-related changes in tissue integrity, and the importance of gentle, progressive approaches. In individuals who are pregnant, certain points are approached with caution, and a practitioner with obstetric experience can determine suitability and optimal timing. For patients with autoimmune or neurologic conditions, acupuncture may modulate immune or neural pathways in ways that complement conventional therapies, yet treatment should always be coordinated with the broader medical team to ensure safety and consistency with overall care goals. Across these populations, patient education, ongoing assessment, and collaborative decision-making are essential elements of a successful acupuncture program.
Practical considerations for maximizing benefits
To derive the most from acupuncture, patients often find it helpful to prepare for sessions with clear goals and to communicate openly about pain patterns, triggers, and activities that influence symptoms. Consistency tends to yield better results, so adhering to a regular treatment schedule, as advised by the practitioner, supports gradual improvement. Hydration, appropriate nutrition, and adequate rest contribute to the body’s capacity to respond to treatment. Following sessions, gentle movement and light stretching can sustain gains, while avoiding sudden, strenuous exertion immediately after treatment protects the body during early recovery. A mindful approach to pain, one that acknowledges both sensory and emotional components, can reinforce the beneficial effects by reducing tension and promoting a calmer nervous system response. In addition, maintaining a shared record of pain scales, functional goals, and quality-of-life measures helps both patient and practitioner track progress and adapt the plan as needed.
Integrating acupuncture with lifestyle changes
Beyond the treatment room, acupuncture is most effective when embedded within broader lifestyle patterns that support nervous system balance and tissue health. Regular physical activity tailored to the individual’s capacity, posture education, and ergonomics can reduce musculoskeletal strain that contributes to chronic pain. Mindfulness practices, such as focused breathing and body awareness, often complement acupuncture by reducing hypervigilance to pain and improving coping strategies. Adequate sleep, balanced nutrition rich in anti-inflammatory components, and stress management techniques create a foundation in which the body can heal and respond to interventions. In this integrated framework, acupuncture serves as a facilitator, helping to normalize the body’s responses so that therapeutic exercises, manual therapies, and other modalities achieve deeper, more sustained benefits.
Personal experiences and cultural considerations
Many patients describe acupuncture as a pathway to reestablish a balanced relationship with their bodies. For some, the ritual and attentiveness of care provide a sense of grounding that reduces anxiety and improves adherence to treatment plans. The subjective nature of pain means that patient narratives—descriptions of relief, changes in sleep quality, and the ability to resume activities previously limited by pain—carry significant weight alongside objective measures. Cultural beliefs surrounding traditional medicine can shape expectations and perceived value, and respectful, open dialogue between patient and practitioner helps align treatment with personal values while maintaining scientific rigor. This human-centered dimension of acupuncture is an important complement to data gathered in trials, illustrating how clinical practice thrives when empathy, competence, and evidence converge.
What the science says about long-term outcomes
When considering long-term outcomes, acupuncture appears to offer sustained benefits for some individuals, particularly when combined with ongoing physical activity, rehabilitation, and healthy lifestyle habits. While not every patient experiences dramatic, lasting change, a subset reports meaningful reductions in pain intensity, improved function, and better quality of life that persist beyond the immediate treatment window. The durability of these effects may relate to ongoing neuromodulation, cumulative exposure to therapeutic point stimulation, and enhancements in coping strategies that reduce the impact of pain on daily living. Recognizing the variability among individuals, clinicians often emphasize patience, regular assessment, and a flexible approach that adapts to evolving symptoms and goals. In research terms, the search for predictors of response continues, with attention to pain phenotype, psychological factors, and comorbidity profiles that help tailor acupuncture to those most likely to benefit.
Closing reflections on a holistic approach to pain relief
Acupuncture represents a bridge between ancient healing wisdom and modern scientific inquiry, offering a pathway that respects the body’s capacity to regulate itself while acknowledging the real burdens that pain imposes on daily life. For many, the experience of receiving careful, attentive care, combined with measurable improvements in pain and function, contributes to a more hopeful and active stance toward recovery. The best outcomes arise when acupuncture is integrated thoughtfully with medical guidance, physical rehabilitation, and lifestyle strategies, forming a cohesive plan that addresses symptom relief, functional goals, and overall well-being. In this light, acupuncture can be seen not merely as a technique for transient discomfort but as a meaningful component of a patient-centered journey toward greater comfort, mobility, and vitality.










